-
PDF
- Split View
-
Views
-
Cite
Cite
Levent Soydan, Ali Aslan Demir, Atadan Tunaci, Frequency of abnormal pulmonary computed tomography findings in asylum seeking refugees in Turkey, International Health, Volume 9, Issue 2, March 2017, Pages 118–123, https://doi.org/10.1093/inthealth/ihw057
Close - Share Icon Share
Abstract
Lungs are particularly vulnerable to both acute infections, including TB, and chronic diseases such as chronic obstructive pulmonary disease, as well as to malignancies, all of which require particular attention during war times in which health conditions are far from optimal.
This retrospective cross-sectional study included 1149 refugees that underwent thoracic computed tomography (CT) for respiratory symptoms between March 2013 and February 2015 in Turkey.
At least one positive CT finding was seen in 231 (20.1%) of the patients. The most common findings were chronic pulmonary changes (n=197, 17.2%), followed by findings suggestive of infections (n=39, 3.4%), and mass/nodular lesions (n=16, 1.4%). The rates of the lesions suggestive of active TB and malignancy were 1.0% (n=11) and 0.7% (n=8), respectively. Age 55–64 years was an independent significant predictor for any CT lesion, chronic changes, mass lesions, and lesions suggestive of malignancy. Age>65 years was predictive of any CT lesion and chronic changes.
The findings of this study indicate the need for implementation of cost-effective screening strategies in refugees, particularly during war times. Screening for TB would improve disease control among both refugees and the host populations. Middle aged and older individuals, in particular, would benefit from more proactive screening tools and strategies for the early diagnosis of pulmonary malignancies and chronic lung diseases.
Introduction
The Syrian civil war has resulted in an increasing number of people fleeing the neighboring countries, which exceeded 4 million by the end of 2015.1 In response to the human right violations and increasing humanitarian needs, particularly from 2012 onwards, Turkey has adopted an ‘open gate’ policy. As a result, it is currently sheltering the highest number of refugees in the region.2 The number of officially registered refugees in Turkey has exceeded 2.2 million,2 with more than 250 000 living in AFAD (Disaster and Emergency Management Agency of the Turkish Government) Temporary Protection Centers.3 New legislation allows refugees to obtain free primary health care services and emergency care from the state hospitals and medical centers.4
War conditions have unfavorable effects on the health and wealth of individuals due to the lack of resources, such as healthy food and water, housing accommodations and healthcare, as well as the increased risk of violence. Forced displacement or migration further complicates the issue, since the provision of basic needs in a short period of time is itself a major challenge, with crowding posing additional health risks. Thus, the physical and mental health of refugees represents a medical challenge and healthcare burden to both governments and healthcare providers, due to extraordinary physical conditions and differences in disease patterns when compared to the host population.
Among refugees, communicable diseases in general, and TB in particular, have been of great research interest. Higher TB rates have been reported among refugees when compared to the host populations.5,6 However, non-communicable diseases have stimulated less interest, although they still represent a challenge for host countries. Several studies have addressed the burdens related to chronic diseases, physical and mental disabilities, and malignancies among refugees in the region.7–12
The lungs are particularly vulnerable to both acute infections, like TB, and chronic diseases. Thoracic computed tomography (CT) is an effective tool to detect structural and inflammatory changes in the lungs, and seems to represent a valuable diagnostic tool for refugees when the findings of the initial diagnostic approaches necessitate further investigation. To date, no study has examined the thoracic CT findings of this high-risk population.
Therefore, this study examined the thoracic CT findings of asylum seeking refugees with respiratory complaints who were admitted to two large clinics in a Turkish metropolis (Istanbul).
Methods
This retrospective study screened the medical files of 1149 refugees seeking asylum in Turkey, who had been referred to the Capa Medical Faculty at Istanbul University or Haydarpasa Numune State Hospital between March 2013 and February 2015 for respiratory symptoms and abnormal chest x-ray findings. The symptoms included cough, weight loss, and/or fever, suggesting pulmonary disease. The patients were initially admitted to shelter camps or primary care facilities for their symptoms, and they were referred to the two tertiary care institutions for further investigation since their chest x-ray findings were abnormal. All of the patients underwent thoracic CT examinations as part of a further diagnostic work up. The referred patients underwent CT examination within one week following their admission. The CT images of the patients were re-examined retrospectively by two radiologists experienced in thoracic CT imaging, and the consensus results were reported. This study protocol was approved by local ethics committee of the Capa Medical Faculty at Istanbul University.
Thoracic CT examination
All of the imaging studies were done at a single imaging center. The thoracic CT imaging ranged from the apex to the base of the lung, including the chest wall and the axillary fossa, and was performed on a 256-detector CT system (Philips ICT 256 Multislice CT, Philips Medical Systems, Veenpluis, The Netherlands) without contrast. The following scan parameters were used: section width 1.5 mm, pitch 0.804, tube voltage 100 kV, tube current 80 mA, display field of view 440 mm, and matrix size 512 × 512. For the image reconstructions, standard and high-resolution reconstruction kernels were used.
Classification of thoracic CT findings
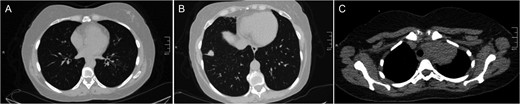
Examples of computed tomography images. (A) bilateral tree-in-bud pattern most prominent in lower lobe of left lung highly suggestive of active TB; (B) lobulated solid mass with spiculated margins in anterior segment of right lower lung highly suggestive of lung cancer; (C) soft tissue density in left lung apex invading upper mediastinum suggestive of pancoast tumor.
Statistical analysis
IBM SPSS Statistics for Windows, Version 21.0. (IBM Corp., Armonk, NY, USA) was used for the analysis of the data, which was presented as numbers (percentages) or the mean±SD, where appropriate. For the comparison of the dichotomous variables, Pearson's χ2 test or Fisher's exact test was used. The Student's t test was used for the independent samples, or the Mann-Whitney U test was used for the comparison of the continuous variables, depending on the normality of the distribution. A logistic regression was used for the multivariate analysis to identify the independent predictor(s) of the lesion types. A p-value less than 0.05 was considered to be an indication of statistical significance.
Results
Table 1 shows the demographic characteristics and lesion distribution of the patients. The mean age was 40.7±15.2 years old (range 14–87), and the male to female ratio was 0.9. Among all of the patients, 231 had at least one abnormal CT finding. The most common findings were chronic changes (n=197, 17.2%), followed by findings suggestive of infections (n=39, 3.4%), and mass/nodular lesions (n=16, 1.4%). Among patients with infection findings, 11 had findings strongly suggestive of active TB (1.0% of all patients). Eight of the mass/nodular lesions were highly suspicious of malignancy (0.7% of all patients). In addition, eight patients (0.7%) had non-pulmonary findings: situs inversus, remnant thymus, hiatal hernia, hydatid liver cyst, pericardial effusion, cardiomegaly and retrosternal goiter.
Distribution of thoracic computed tomography findings by demographical characteristics and year of admission
| . | n . | Any finding n (%) . | Chronic changes n (%) . | Infection findingsa n (%) . | TBCb n (%) . | Mass/nodular lesionsc n (%) . | Malignancyd n (%) . |
|---|---|---|---|---|---|---|---|
| All patients | 1149 | 231 (20.1) | 198 (17.2) | 39 (3.4) | 11 (1.0) | 16 (1.4) | 8 (0.7) |
| Gender | |||||||
| Female | 543 | 112 (20.6) | 97 (17.9) | 16 (2.9) | 6 (1.1) | 6 (1.1) | 4 (0.7) |
| Male | 606 | 119 (19.6) | 101 (16.7) | 23 (3.8) | 5 (0.8) | 10 (1.7) | 4 (0.7) |
| Year of admission | |||||||
| 2013 | 514 | 106 (20.6) | 93 (18.1) | 20 (3.9) | 7 (1.4) | 7 (1.4) | 3 (0.6) |
| 2014–2015 | 635 | 125 (19.7) | 105 (16.5) | 19 (3.0) | 4 (0.6) | 9 (1.4) | 5 (0.8) |
| Age group | |||||||
| <55 | 925 | 144 (15.6) | 121 (13.1) | 28 (3.0) | 7 (0.8) | 9 (1.0) | 3 (0.3) |
| 55–64 | 123 | 40 (32.5) | 33 (26.8) | 6 (4.9) | 3 (2.4) | 5 (4.1) | 4 (3.3) |
| >64 | 101 | 47 (46.5) | 44 (43.6) | 5 (5.0) | 1 (1.0) | 2 (2.0) | 1 (1.0) |
| . | n . | Any finding n (%) . | Chronic changes n (%) . | Infection findingsa n (%) . | TBCb n (%) . | Mass/nodular lesionsc n (%) . | Malignancyd n (%) . |
|---|---|---|---|---|---|---|---|
| All patients | 1149 | 231 (20.1) | 198 (17.2) | 39 (3.4) | 11 (1.0) | 16 (1.4) | 8 (0.7) |
| Gender | |||||||
| Female | 543 | 112 (20.6) | 97 (17.9) | 16 (2.9) | 6 (1.1) | 6 (1.1) | 4 (0.7) |
| Male | 606 | 119 (19.6) | 101 (16.7) | 23 (3.8) | 5 (0.8) | 10 (1.7) | 4 (0.7) |
| Year of admission | |||||||
| 2013 | 514 | 106 (20.6) | 93 (18.1) | 20 (3.9) | 7 (1.4) | 7 (1.4) | 3 (0.6) |
| 2014–2015 | 635 | 125 (19.7) | 105 (16.5) | 19 (3.0) | 4 (0.6) | 9 (1.4) | 5 (0.8) |
| Age group | |||||||
| <55 | 925 | 144 (15.6) | 121 (13.1) | 28 (3.0) | 7 (0.8) | 9 (1.0) | 3 (0.3) |
| 55–64 | 123 | 40 (32.5) | 33 (26.8) | 6 (4.9) | 3 (2.4) | 5 (4.1) | 4 (3.3) |
| >64 | 101 | 47 (46.5) | 44 (43.6) | 5 (5.0) | 1 (1.0) | 2 (2.0) | 1 (1.0) |
a Findings suggestive of acute infection including active TB.
b Only the findings strongly suggestive of active TB.
c Mass or nodular lesions, either benign or malignant.
d Only the findings strongly suggestive of malignancy.
Distribution of thoracic computed tomography findings by demographical characteristics and year of admission
| . | n . | Any finding n (%) . | Chronic changes n (%) . | Infection findingsa n (%) . | TBCb n (%) . | Mass/nodular lesionsc n (%) . | Malignancyd n (%) . |
|---|---|---|---|---|---|---|---|
| All patients | 1149 | 231 (20.1) | 198 (17.2) | 39 (3.4) | 11 (1.0) | 16 (1.4) | 8 (0.7) |
| Gender | |||||||
| Female | 543 | 112 (20.6) | 97 (17.9) | 16 (2.9) | 6 (1.1) | 6 (1.1) | 4 (0.7) |
| Male | 606 | 119 (19.6) | 101 (16.7) | 23 (3.8) | 5 (0.8) | 10 (1.7) | 4 (0.7) |
| Year of admission | |||||||
| 2013 | 514 | 106 (20.6) | 93 (18.1) | 20 (3.9) | 7 (1.4) | 7 (1.4) | 3 (0.6) |
| 2014–2015 | 635 | 125 (19.7) | 105 (16.5) | 19 (3.0) | 4 (0.6) | 9 (1.4) | 5 (0.8) |
| Age group | |||||||
| <55 | 925 | 144 (15.6) | 121 (13.1) | 28 (3.0) | 7 (0.8) | 9 (1.0) | 3 (0.3) |
| 55–64 | 123 | 40 (32.5) | 33 (26.8) | 6 (4.9) | 3 (2.4) | 5 (4.1) | 4 (3.3) |
| >64 | 101 | 47 (46.5) | 44 (43.6) | 5 (5.0) | 1 (1.0) | 2 (2.0) | 1 (1.0) |
| . | n . | Any finding n (%) . | Chronic changes n (%) . | Infection findingsa n (%) . | TBCb n (%) . | Mass/nodular lesionsc n (%) . | Malignancyd n (%) . |
|---|---|---|---|---|---|---|---|
| All patients | 1149 | 231 (20.1) | 198 (17.2) | 39 (3.4) | 11 (1.0) | 16 (1.4) | 8 (0.7) |
| Gender | |||||||
| Female | 543 | 112 (20.6) | 97 (17.9) | 16 (2.9) | 6 (1.1) | 6 (1.1) | 4 (0.7) |
| Male | 606 | 119 (19.6) | 101 (16.7) | 23 (3.8) | 5 (0.8) | 10 (1.7) | 4 (0.7) |
| Year of admission | |||||||
| 2013 | 514 | 106 (20.6) | 93 (18.1) | 20 (3.9) | 7 (1.4) | 7 (1.4) | 3 (0.6) |
| 2014–2015 | 635 | 125 (19.7) | 105 (16.5) | 19 (3.0) | 4 (0.6) | 9 (1.4) | 5 (0.8) |
| Age group | |||||||
| <55 | 925 | 144 (15.6) | 121 (13.1) | 28 (3.0) | 7 (0.8) | 9 (1.0) | 3 (0.3) |
| 55–64 | 123 | 40 (32.5) | 33 (26.8) | 6 (4.9) | 3 (2.4) | 5 (4.1) | 4 (3.3) |
| >64 | 101 | 47 (46.5) | 44 (43.6) | 5 (5.0) | 1 (1.0) | 2 (2.0) | 1 (1.0) |
a Findings suggestive of acute infection including active TB.
b Only the findings strongly suggestive of active TB.
c Mass or nodular lesions, either benign or malignant.
d Only the findings strongly suggestive of malignancy.
Table 1 also shows the distribution of the CT findings by age, gender and year of admission. The gender distribution was not significantly different among the patients with or without chronic changes, infection findings, findings suggestive of TB, mass/nodular lesions, and findings suggestive of malignancy (p>0.05 for all). The frequency of each lesion type was similar across the two time frames (i.e., 2013 vs 2014–2015) (p>0.05 for all). The mean age of patients with at least one CT abnormality was significantly higher than in patients with normal CT findings (48.5±17.4 vs 38.8±13.9 years old, p<0.001). In addition, patients with chronic changes (49.0±17.7 vs 39.0±14.0 years old, p<0.001), infectious lesions (46.4±16.9 vs 40.5±15.1 years old, p=0.024), lesions suggestive of malignancy (52.3±14.2 vs 40.6±15.2 years old, p=0.027) and TB (51.2±17.1 vs 40.6±15.1 years old, p=0.036) were significantly older when compared to patients without these respective lesions.
According to the multivariate analysis, being in the age group of 55–64 years was an independent significant predictor for any CT lesion, chronic changes, mass lesions, and lesions suggestive of malignancy. However, being in the higher age group was predictive of any CT lesion and chronic changes. The odds ratios and confidence intervals are shown in Table 2.
Age groups as predictors of computed tomography lesions
| . | Odds ratio (95% CI) . | p-value . |
|---|---|---|
| Age 55–64 | ||
| Any lesion | 2.6 (1.7–4.0) | <0.001 |
| Chronic changes | 2.4 (1.6–3.8) | <0.001 |
| Mass/nodular lesion | 4.5 (1.5–13.6) | 0.008 |
| Malignancy | 10.2 (2.3–46.5) | 0.003 |
| Age>64 | ||
| Any lesion | 4.7 (3.1–7.3) | <0.001 |
| Chronic changes | 5.1 (3.3–8.0) | <0.001 |
| . | Odds ratio (95% CI) . | p-value . |
|---|---|---|
| Age 55–64 | ||
| Any lesion | 2.6 (1.7–4.0) | <0.001 |
| Chronic changes | 2.4 (1.6–3.8) | <0.001 |
| Mass/nodular lesion | 4.5 (1.5–13.6) | 0.008 |
| Malignancy | 10.2 (2.3–46.5) | 0.003 |
| Age>64 | ||
| Any lesion | 4.7 (3.1–7.3) | <0.001 |
| Chronic changes | 5.1 (3.3–8.0) | <0.001 |
Age groups as predictors of computed tomography lesions
| . | Odds ratio (95% CI) . | p-value . |
|---|---|---|
| Age 55–64 | ||
| Any lesion | 2.6 (1.7–4.0) | <0.001 |
| Chronic changes | 2.4 (1.6–3.8) | <0.001 |
| Mass/nodular lesion | 4.5 (1.5–13.6) | 0.008 |
| Malignancy | 10.2 (2.3–46.5) | 0.003 |
| Age>64 | ||
| Any lesion | 4.7 (3.1–7.3) | <0.001 |
| Chronic changes | 5.1 (3.3–8.0) | <0.001 |
| . | Odds ratio (95% CI) . | p-value . |
|---|---|---|
| Age 55–64 | ||
| Any lesion | 2.6 (1.7–4.0) | <0.001 |
| Chronic changes | 2.4 (1.6–3.8) | <0.001 |
| Mass/nodular lesion | 4.5 (1.5–13.6) | 0.008 |
| Malignancy | 10.2 (2.3–46.5) | 0.003 |
| Age>64 | ||
| Any lesion | 4.7 (3.1–7.3) | <0.001 |
| Chronic changes | 5.1 (3.3–8.0) | <0.001 |
Discussion
This study examined the thoracic CT findings of symptomatic asylum seeking refugees. To the best of our knowledge, this was the first study to specifically review the thoracic CT findings of a refugee population. The findings indicate the need for important public health actions during humanitarian emergencies.
TB seems to escalate among populations affected by crises, including immigration, war and natural disasters, with a 2-fold or greater increase in the prevalence/incidence rates when compared to the reference populations.13 Such conditions are accompanied by a shortage of healthcare resources and infrastructure for the diagnosis, treatment and follow-up of the cases, a lack of medication, and unhealthy living conditions, including crowding and inadequate sanitation.
TB cases among Syrian refugees were reviewed in a recent study from Jordan, where approximately 600 000 refugees had been hosted by the end of 2014.5 An active public health strategy, including screening, increasing awareness, and providing efficient treatment, was implemented, with the coordination of national and international organizations. The initial results showed an improved detection of index cases, which may translate into better disease control over the long term, since more than 85% of newly diagnosed cases can be cured.5 In that study, the prevalence among the refugees was twice as high as that in the host population. Similar increases in the TB burden have been observed among other displaced people during wartimes, including the Iraq, Bosnia Herzegovina and Georgia conflicts.5,14,15 A recent Italian study conducted on a large population of migrants revealed a 0.1% active TB prevalence, while the corresponding figure for the host country was below 0.01%.16,17
Our study found lesions suspicious of TB among almost 1% of refugees (n=11) with respiratory symptoms, but the true prevalence in our study group may have been even higher. In our situation, only the symptomatic cases were worked up, but patients with normal chest x-rays may also harbor the disease. The reported prevalence of TB in the overall Turkish population was 21/100 000 in 2011, although the incidence of TB has been decreasing over the years.18 The 1% rate found in our study population may not represent the true prevalence, but it is still higher than the prevalence of the host country, and thus points out the need for the implementation of active cost-effective screening strategies and the further investigation of symptomatic/suspicious cases. Therefore, in host countries with a low prevalence of TB, it may become an issue to be considered.
The refugees in some host countries do not undergo routine TB screenings and/or surveillance programs, so active TB cases can only be detected when they are admitted for a specific complaint, as in our study, or when they are screened for specific signs suggestive of TB. However, increased detection and active treatment may be possible with effective screening upon arrival, followed by specific TB surveillance programs aimed at refugees.5 Such a strategy could potentially prevent further health problems, including the increased transmission and emergence of treatment resistant cases. It is particularly challenging to diagnose TB in children19; therefore, younger age groups would also benefit from effective screening strategies.
Two other notable findings of this study were the high frequency of chronic pulmonary changes (n=197, 17.2%), and the relatively high frequency of lesions suspicious of infection and malignancies (particularly among refugees 55–64 years old, n=55, 4.8%), mainly lung cancer, among this subgroup of patients with positive CT findings. In the multivariate analysis, this specific age range emerged as high-risk group, with an almost 10-fold increase in the risk normally expected for pulmonary malignancies. Given the high tobacco consumption in the region,20–22 this is not an unusual finding, and it is in line with the findings of several studies that have examined malignant conditions in a refugee setting in particular. For example, Spiegel et al. examined the retrospective data of all refugees from Jordan or Syria who applied for the treatment of any disease, and extracted the cancer data.7 Of the 1989 applicants, 511 (25.6%) had cancer, and the mean age at the time of admission for cancer was 49 years. Breast cancer was the most frequently identified cancer (20.4%), while 15 cases of lung cancer were diagnosed, constituting 2.9% of all patients.7 Another study examined the cancer profile of Afghani refugees in Iran, and found a 13.3% cancer frequency among the referrals for any reason, with 25% of all cancers being gastrointestinal system malignancies.23 In that study, only 4.4% of all of the cancers were pulmonary malignancies, constituting only 0.5% of all referrals. Another study screened US-bound Iraqi refugees for chronic conditions, including cancer,12 and that study population included Iraqi refugees screened before their arrival, rather than applicants or referrals for a specific reason. Among the 18 990 refugees screened, 97 had been previously diagnosed or were currently receiving treatment for cancer (0.5%); however, specific screening for lung cancer was not conducted (although 19.3% were smokers), so the lung cancer data were not available.12 The findings of the latter study may be an indication of an underestimation of malignant thoracic conditions in a refugee setting.
In Turkey, the estimated lung cancer incidence figures range between 42 to 69/100 000 for men and 5 to 8/100 000 for women.24 One previous Turkish study estimated the prevalence of incidental pulmonary findings in 1206 patients undergoing CT coronary angiography, and three cases of lung cancer (0.24%) and one case of breast cancer (0.08%) were detected.25 These figures may provide an idea of the lung cancer prevalence of the host population; however, a direct comparison with the 0.24% frequency found among the refugees in this study would be misleading. In the latter, all of the patients had pulmonary symptoms, and the lesions suggestive of malignancy were not confirmed clinically.
Given the high prevalence of chronic structural changes and the relatively high rate of lesions suspicious of malignancy among our patients, as well as the high consumption of tobacco in the region, lack of advanced diagnostic facilities in the host country, and high prevalence of previously reported pulmonary malignancies, our findings indicate the need for more proactive screening and diagnostic approaches for these particular age groups.
Non-communicable diseases have been largely neglected in the refugee setting, since they usually do not emerge as emergencies. However, chronic conditions in general, and malignances in particular, represent major challenges in terms of life expectancy, morbidity, life quality over the long term, and substantial healthcare costs for the host country. The high prevalence of chronic structural changes in the lungs must be addressed, and necessary management strategies should be aimed at chronic respiratory diseases.
The main limitations of this study were the lack of clinical confirmation of the imaging findings and the lack of a control group, which would have provided information about the host population. In addition, a detailed clinical evaluation at the initial entry point to the country was not available, due to limited availability of health services on the border. Another potential limitation was the retrospective nature of the study. Moreover, the study population consisted of applicants with pulmonary symptoms, rather than individuals screened for pulmonary diseases. However, the time lag between the initial referral of the symptomatic patient and the CT examination was relatively short, thus reflecting a good temporal association between the symptoms and imaging findings. Although the true incidence or prevalence could not be generated, and the figures can only be used for guiding further efforts, the findings seem to be sufficient to delineate important healthcare issues to address and guide cost-effective preventive, diagnostic and management strategies.
CT imaging has a high diagnostic value in detecting a wide range of pulmonary pathologies, and is particularly beneficial when the initial diagnostic or screening approaches are suggestive of pulmonary disease. It has high sensitivity and specificity for lung cancer (94% and 73%, respectively) when compared to a chest x-ray (74% and 91%, respectively).26 Although bacteriological and/or histological examinations are required to confirm a TB diagnosis,27 a chest CT is sensitive in the detection of cavitation, hilar and mediastinal lymphadenopathy, the endobronchial spread and complications in the course of the disease. It may identify the foci of the disease, particularly in cases of miliary TB, and may be beneficial in the differential diagnosis and tuberculous activity assessment.28–30 In addition, a CT is valuable in the diagnosis of diffuse lung diseases, including infections.31 However, it is worth noting that the main focus of the findings of this study was the frequency of lung lesions among asylum seeking refugees, necessitating a more comprehensive use of the currently recommended cost-effective screening tools and strategies, rather than proposing CT imaging as an initial screening tool in this setting. Our currently available radiological data provides evidence to draw attention to this public health issue; however, CT imaging is far from being an initial screening tool, considering its relatively high cost and low availability.
Considering the importance of the early detection of pulmonary diseases among refugees, particularly TB and malignant conditions, a proactive strategy needs to be implemented. If a pre-departure medical record is available, it should be reviewed carefully. Upon arrival, a thorough medical history of each refugee should be obtained, preferably by administering a questionnaire.16 In addition, the proactive screening of all refugees for active TB and malignancies with chest x-rays seems to be a cost-effective strategy, since it is a relatively cheap and readily available imaging technique when compared to CT imaging. In Turkey, the cost of a chest x-ray is approximately US$7 for the patient and US$5 for the healthcare provider. The corresponding figures for a thoracic CT examination are US$50 and US$35, respectively. The individuals who present with, or report a history of, TB, those with a history of contact with cases of active pulmonary TB, and those who report clinical signs and symptoms of TB during the screening process should also be referred for sputum investigations (direct smear and culture). A purified protein derivative (PPD) test (Mantoux tuberculin skin test) seems to be less reliable in this setting, because of the high possibility of prior exposure to the pathogen. In the few unresolved cases, a referral for a thoracic CT may be necessary to clarify the condition, since a CT has high sensitivity and specificity for all pulmonary lesions, including malignancies.
Conclusions
TB, lung cancer, and chronic pulmonary changes seem to represent important health problems among asylum seeking refugees. The proactive and effective screening of refugees for active TB, thoracic malignancies (particularly among the middle aged symptomatic refugee population), and chronic pulmonary diseases (particularly among older individuals) seems plausible. Providing easy and effective access to healthcare services and screening of all refugees with physical and chest X-ray examinations may represent a cost-effective strategy.
Authors’ contributions: LS conceived the study; LS, AAD and AT and designed the protocol; LS, AAD and AT reviewed and interpreted CT images; LS drafted the manuscript, AAD and AT critically revised the manuscript for intellectual content. All authors read and approved the final manuscript. LS is guarantor of the paper.
Funding: None.
Competing interests: None declared.
Ethical approval: Ethical approval was provided by local ethics committee of Capa Medical Faculty, Istanbul University.
References
- chronic obstructive airway disease
- computed tomography
- lung
- lung diseases
- cancer
- cost effectiveness
- chronic disease
- psychiatric hospital
- middle-aged adult
- refugees
- signs and symptoms, respiratory
- tuberculosis
- wars
- infections
- mass lesion
- older adult
- chest ct
- early diagnosis
- host (organism)
- active tuberculosis




Comments